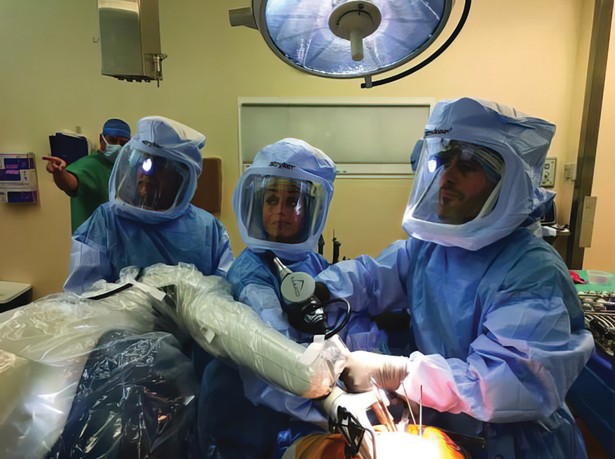
For Dr. Christopher Gorczynski, an orthopedic surgeon at Columbia Memorial Health (CMH) in Hudson, a highly skilled robot surgical assistant isn’t a distant science fiction dream—it’s an exciting reality in the operating room. In 2017, CMH invested in the Mako Robotic Arm, a cutting-edge technological unit that helps orthopedic surgeons like Dr. Gorczynski plan and perform partial and total knee replacements and total hip replacements with exceptional accuracy.
The increased precision the robotic arm provides allows surgeons to preserve healthy bone and protect soft tissue and ligaments, resulting in better health outcomes like easier recovery and rehabilitation, and a more stable, long-lasting joint prosthesis that is a much better fit to the patient’s individual anatomy. As joint replacement surgery becomes increasingly common, the technological advance of the Mako Robotic Arm is helping patients obtain more predictable outcomes.
“The goal has always been to make a joint replacement feel more natural to patients, to feel like they’ve never had surgery,” says Dr. Gorczynski. There’s a metric orthopedic surgeons use, known as “the forgotten joint score,” a reference to the reconstructed joint’s imperceptibility during daily life. Achieving such a goal, however, hasn’t always been easy. “Historically it’s been an issue because no matter how skilled the surgeon, manual reconstruction of a joint may not have been as accurate as they would like,” he says.
That’s because prior to the introduction of the robotic arm, a surgeon would align joint replacements manually using very simple, decades-old alignment guides. Soft tissue tension was estimated manually, and once bone cuts were made, additional adjustment was not easily or accurately done.
Now, with the help of the Mako Robotic Arm, those issues are a relic of the past.
The robotic arm helps the surgeon achieve a better reconstruction through three key pieces of its software design—3D CT-based planning, AccuStop haptic technology, and real-time data analytics.
Before entering the operating room, the surgeon uses a CT scan of the patient’s joint to 3D-model the reconstruction and create a personalized surgical plan based on each patient’s specific diagnosis and unique anatomy. During the operation, the surgeon controls the robotic arm, which uses its AccuStop technology to prevent anything but the precise plan from being executed. And using the real-time information that the robotic arm provides, the surgeon can virtually stress test the prosthesis and make any necessary adjustments.
That means Dr. Gorczynski can implant a hip or knee joint prosthesis within a millimeter and a degree of intended plan every time. “No surgeon anywhere can do this consistently using manual tools,” he says. “Since we began doing joint replacement robotically, it has exceeded my expectations with regard to accuracy of reconstruction, and it’s been so rewarding to offer this to the community.”