Dear reader,
First off: Don’t panic.
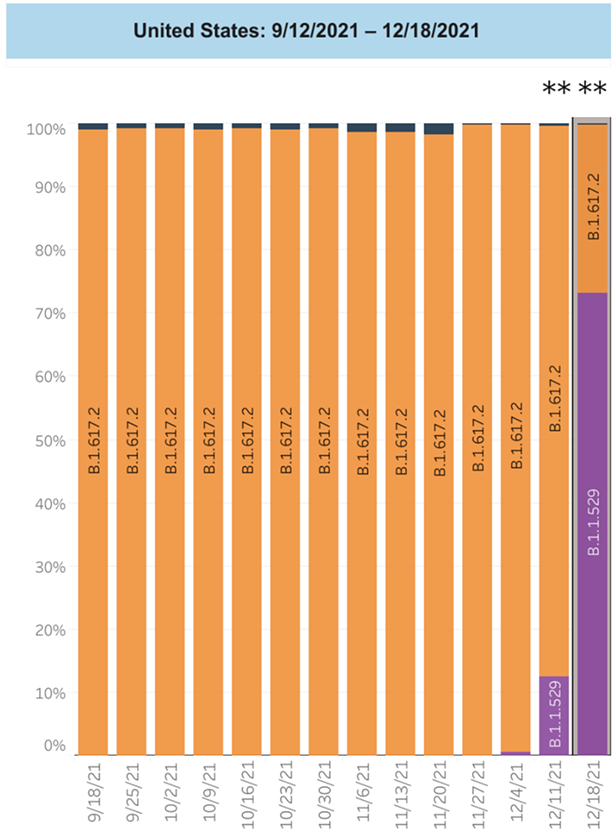
With great swiftness, over the past week the Omicron variant has become the dominant form of COVID-19 in New York State and the US. As of December 18, the CDC estimates that Omicron made up 73.2 percent of the cases in the nation, a figure that is already being eclipsed.
One thing I’ve learned over and over again through reporting on the pandemic is that large areas like a country, or even a state, are too broad a lens to see what’s going on in communities. Omicron is driving a surge in New York State’s overall case count, but it’s not yet dominant in all of the state’s 62 counties. (It almost certainly will be soon.)
That means that for many of us in upstate New York, our already high local infection levels are going to go up sharply. By how much, it’s impossible to say. But whatever your local odds are now of getting infected by a dinner or a holiday party or a public-facing job, expect them to rise steeply over the next month or so before falling quickly. In South Africa, the Omicron surge began in late November, and seems to have already passed its peak.
If you live somewhere in the Hudson Valley and Catskills, this guide is for you. And no matter where you are, we hope you’ll find something useful. —Lissa Harris
What’s Different About Omicron?
It spreads more easily. Omicron is now the second-most contagious human virus in the world, second only to measles. In areas with local Omicron spread, cases will double every two or three days.
Which brings us to the next point:
Your mask probably isn’t good enough. The increased transmissibility of Omicron makes it much more likely to get around a cloth or surgical mask. N95 and KN95 masks provide more protection, but they can be difficult to find, and some online retailers are pushing counterfeits. The New York Times has a recent guide to some of the better options. Facial hair will interfere with the fit of an N95 mask. Another option that’s somewhat better than a non-N95 mask alone is layering a surgical mask under a close-fitting cloth one.
It moves faster through the body. The average time from infection to symptoms was about five days for the Alpha variant, and four for Delta. Omicron infections are clocking in at an average of around three days from infection. That’s bad news for contagiousness and for testing effectiveness, but it could have a silver lining: It might mean we can safely reduce the length of isolation and quarantine, already down to 10 days from the CDC’s original 14.
It appears to be less lethal than Delta—but maybe only for those who have already been infected or vaccinated. Omicron cases in South Africa, where the variant struck early and hard at a mostly unvaccinated population, have had a lower hospitalization rate than the Delta variant. But almost all of the people who got Omicron in South Africa had already recovered from Delta, and the population is younger overall than that of the US. Data now coming from the UK and Denmark will give a better picture of what Omicron infection means for different populations.
Vaccines help, but they don’t stop it from getting in the door. If you’re vaccinated with two doses and a booster of an mRNA vaccine—Pfizer or Moderna—you should have some level of protection against being infected by Omicron; recent studies have found higher rates of protection from Moderna. The jury’s still out on how well people who have had one shot of the J&J vaccine and an mRNA booster are protected. Neither a two-dose course of an mRNA vaccine nor immunity from previous infection offers much protection against becoming infected with Omicron.
The story is very different when it comes to hospitalization and death. A regular course of vaccination still offers high levels of protection against the worst outcomes, even without a booster dose. That’s because although the antibody protection that is the first line of defense against infection wanes over time, the slower T-cell response that mobilizes to fight off an infection is more durable. Think of it this way: If your body is a bank and Omicron is a robber, vaccines might not stop it from getting through the front door and pilfering the teller’s desk, but they will heavily fortify the vault.
Prepare to test positive. A lot of people who have been vaccinated or who have already had COVID-19, or both, will come down with Omicron in the next few weeks or months. This variant’s sheer infectiousness is going to lead to a lot of breakthrough cases, most of them probably unpleasant but not life-threatening. That doesn’t mean infection is inevitable, or that it doesn’t help to manage your risk, but you may want to be mentally and logistically ready to get sick and have to isolate for 10 days, possibly from other people in your household.
Data will get worse. Omicron is already pushing the limits of the US testing and tracing infrastructure, and in places where testing is already inaccessible, it will overwhelm them fast. That means there will be a lot of infections that go unreported, which will make local case numbers seem lower than they are in reality, and also make it more difficult for health officials to predict how fast hospitalizations will rise.
Finally, and importantly:
Omicron is a disrupter. If you’re in a group that tends not to have bad COVID outcomes, or you have a high tolerance for personal risk, you may be willing to do riskier things, even knowing that it’s likely you’ll be infected. The level of risk that feels right will be different for everyone. But one thing to keep in mind: With an airborne virus that’s almost as contagious as measles and tends to double local case counts every day or two while it is peaking, other risks also rise. Health care becomes less available and less effective as workers get sick or exhausted from the workload. Logistical systems and services that work fine at a lower level of community infection may become too frayed to function well.
Getting sick during a time of widespread community disruption might be more difficult and dangerous than it would be during a downturn in local infection rates. If you get sick during a steep surge in cases, you may not be able to get tested, or your test results may be delayed so much that they won’t be useful.
What’s the Same?
All the stuff we’ve been doing still reduces Omicron risk. Masking, ventilation, vaccines, smaller gatherings, socializing outdoors: It all helps reduce risk of infection. Just not as much as it used to.
If you want to prevent infection, a layered approach with multiple strategies (like vaccinating and also masking indoors) will provide more protection than any one strategy alone.
Cleaning surfaces still doesn’t do much. This was something scientists were wrong about early on. We’ve known for awhile now COVID-19 is airborne and that surface transmission is vanishingly rare, but “hygiene theater” has persisted in a lot of businesses and indoor spaces. Good ventilation (or air filtration) is a lot more effective at slowing transmission.
Hospitalizations and deaths don’t reflect current cases. Current hospitalizations are mostly from infections that began a week ago, or longer. Current deaths are mostly from even older cases. The recent infections that are now driving case rates to new records in New York won’t start to show up in the more serious indicators for at least a week or two.
For most, a bout with Omicron won’t be life-threatening, but there are a lot of vulnerable people. Politicians at the state and federal levels are vowing not to let Omicron shut down work and school, emphasizing that people who have been vaccinated and boosted are at low risk from Omicron. But that group only makes up a small percent of New York’s population, and in many places, much less. Those who are fully vaccinated will fare better than the unvaccinated, on average. But the unvaccinated include all children under the age of five, along with many others in all other age groups. Many pregnant people are unvaccinated. In nursing homes and group homes, many vulnerable residents have been vaccinated but not boosted. Vaccination rates are low in prisons. Immunocompromised people and those with underlying medical issues may be highly vulnerable to Omicron even if they have been vaccinated.
Rapid tests can help make events safer. Much ado has been made about the fact that rapid tests aren’t as accurate at diagnosing a case of COVID-19 as PCR tests—and it’s true, they’re not. What they are very good at is determining whether someone is currently contagious. Taking a rapid test immediately before a gathering isn’t a perfect guarantee that you won’t spread Omicron to your friends and family, but if you have enough virus in your system to be contagious, you are very likely to test positive.
We still don’t know much about long COVID. Researchers are working on it, but it’s a slow riddle to solve.
New Plans and New Resources
Note: This list is a snapshot in time as of December 23. More resources may become available quickly, and some of those listed here may disappear without notice. In general, if there is something you need urgent help with, check with your local community institutions to see if they are working on it: your county or city public health department; your town, village, city, or county government; social services agencies and organizations; local libraries and places of worship; food banks; local nonprofits and economic development organizations; and other community resources. If they can’t help you, they might know who can.
Federal
President Joe Biden announced on Tuesday, December 21, that the White House will buy 500 million rapid tests and send them for free to US residents who sign up on a website to receive them, starting in January. It’s a quick turnaround for the Biden administration, whose press spokesperson Jen Psaki publicly scoffed at the idea of sending tests to households just a couple of weeks ago. The website has not yet been announced, and requiring people to sign up online for the tests will present access barriers for people who don’t have internet access or are not fluent with digital tools.
The Biden administration is also mobilizing federal funds and resources to help states respond. In New York, the feds are deploying staffed ambulances upstate, and setting up new testing sites statewide.
Federal student loan repayment will remain suspended until May 1.
New York State
The state’s new winter surge plan, announced by Governor Kathy Hochul on Monday, December 20, has already begun to go into effect. County health departments are receiving new shipments of home tests from the state, some of which have already been distributed. Schools and state mass vaccination sites are also receiving tests. The state is launching seven new vaccination sites, and plans to distribute six million masks to counties. Hochul’s new Department of Health Commissioner, Mary Bassett (who tested positive for COVID-19 on Monday), has vowed that this administration would have a better relationship with county governments and health officials than ex-governor Andrew Cuomo’s did.
On Wednesday, December 22, Governor Hochul signed a package of new pandemic legislation. Falsification of a vaccine card is now a class D felony. Schools will have increased access to student immunization data. The state Department of Health will conduct a study of how the pandemic has affected medical care, with the goal of improving access, especially in “health deserts.” The Department of Financial Services will also study the pandemic’s impact on banking and small businesses in areas underserved by banking.
Hochul declared a statewide mask mandate in effect as of December 10 for all public indoor spaces that do not require proof of vaccination, but many counties have announced that they will not enforce it. To some extent, that’s a moot point, because neither the state nor local governments have much capacity to enforce masking at any scale, but the pushback from local governments may leave residents confused as to whether they have to mask or not.
Counties that participate in enforcement can apply for either $1 or $2 million, depending on county size, of $65 million in state funds set aside on December 20 to help county health departments cope with new enforcement demands.
Elective surgeries have been temporarily halted as of December 9 at 32 upstate hospitals whose capacity is being strained by increased COVID-19 hospitalizations and staff loss. More hospitals may restrict elective procedures or patient visitation as they become stressed.
Local
A good resource for keeping an eye on local risk is the CDC’s map of community transmission in the US, which allows you to choose your county to see where local rates of infection, hospitalization, death, and vaccination currently stand. As of December 23, case rates in the lower Hudson Valley are starting to go vertical, with both Rockland and Westchester showing increases of more than 100 percent in the case rate over the past week, but rates in Mid-Hudson and Catskills counties are either on a slow decline or just beginning to shoot up. That will change fast as Omicron gains more of a local foothold.
A wide variety of local and regional data is available through New York State’s COVID-19 data page. State data might not always agree with CDC data because of timing differences and differences in how agencies collect and report raw data coming in from healthcare providers and other sources.
Your county health department may have rapid tests, masks, or other resources; state agencies are currently working to get resources into the hands of local authorities.
State and local officials have vowed to keep schools open, but school shutdowns are already being declared locally in places where the logistics of keeping them open are becoming overwhelming. Keep in touch with your local school district about changes, which may be announced abruptly.
LOWER HUDSON VALLEY
County coronavirus pages: Rockland, Westchester, Putnam
County vaccine pages: Putnam
Rockland County will share details on the distribution of home tests to county residents soon, County Executive Ed Day said in a Monday statement. The county is urging New York State to reopen the state vaccination site at the Anthony Wayne Recreation Center.
“We have seen now in the last few days an absolute explosion in the number of positive cases,” Westchester County Executive George Latimer said during a regular weekly COVID-19 update given on Monday from his home, where he was still recovering from a COVID-19 infection. Joining in digitally was Deputy County Executive Ken Jenkins, who was also isolating due to a positive test.
Westchester County has offered New York State the use of the county center and Glen Island as mass vaccination sites again, Latimer said, and county officials will continue to offer vaccination and tests at the county center. The county is also distributing masks to municipalities, businesses, and local organizations.
Westchester officials are in a tough position on mask enforcement, Latimer said. “It is a difficult mandate to maintain. And for those people who are vaccinated and are very adamant that other people wear masks and be vaccinated: We have a number of people who feel the exact opposite,” he said. “They’re aggressively unvaccinated, unmasked, and do not choose to do anything unless it's at a point of physical force. We want to avoid having that kind of confrontation in the society right now, with us divided already as it is with philosophical camps.”
As of December 23, Putnam County had not made any pandemic-related announcements on their website since the 14th, but they do have a press release about cute animals at the Tilly Foster Farm.
MID-HUDSON VALLEY
County coronavirus pages: Orange, Dutchess, Ulster, Columbia
County vaccine pages: Dutchess, Ulster, Columbia
Ulster County is ahead of the curve on giving home tests to local residents: County Executive Pat Ryan announced on December 14, before the current state push to get tests to counties was announced, that residents would be able to pick up rapid tests at multiple locations starting December 20. Check with your town or village to see where tests are available.
Dutchess County Executive Marc Molinaro announced Wednesday that home test kits and K95 masks will be given to every municipality in the county. Masks and tests will be made available to local residents and businesses. Check with your town or village to see where tests will be made available.
Orange County Executive Steve Neuhaus gives weekly updates on the pandemic via his Facebook page, which can be watched if you have a Facebook account.
“We’re pretty slammed,” said Columbia County Health Director Jack Mabb in a press release on December 17. Another release on the 21st announced that 26 county residents were currently hospitalized.
CATSKILLS
County coronavirus pages: Sullivan, Delaware, Greene, Schoharie
County vaccine pages: Sullivan, Delaware, Greene, Schoharie
None of the Catskills counties have issued recent press releases about Omicron plans as of December 23. Stay tuned to county government and health department websites and Facebook pages for updates, and to see if tests, masks, or other resources will be made available to the public.